Author’s Note: This is the third installment in an ongoing series meant to introduce the Postural Restoration Institute and the concepts that it teaches, as well as how to integrate them into training and rehab. If you missed either of the first two installments, you can click here for Part 1 and here for Part 2 to give those a read. In this installment, I’ll move from the neurological and biochemical/molecular underpinnings of PRI’s methodology discussed in Part 1 and Part 2, respectively, to the more palpable anatomical component, including the common postural and movement patterns that the PRI model describes. The integration of these concepts into training and rehab programs will be covered in greater detail in Part 4.
The First Commandment of PRI: Thou Shalt Not Consider Humans to Be Inherently Symmetrical Beings
Take a look at Leonardo da Vinci’s world-famous Vitruvian Man and you’ll see what most people take for granted: humans are symmetrical beings. After all, we have two arms that look the same, two legs that look the same, and if you cut us down the middle the two halves would appear to mirror each other. I’m no geometry whiz, but that sounds pretty damn symmetrical to me!
The fact is, however, we are not perfectly symmetrical, and if we inspect this claim in some detail it’s really not that hard to see. Take this project, for example, where they cut pictures of peoples’ faces in half and then remade complete faces using each half as a mirror-image for it’s new complementary half. Notice a difference? It’s actually quite surprising–almost all of the people look noticeably different when you use one side of their face to generate a mirror image than does the same procedure with the other side! If you more closely inspect other areas of the human body, you’ll find similar patterns. And that’s really what the practical component of PRI is: identifying and correcting patterns of posture, movement, and muscle activity.
Before I delve into the nitty-gritty, I want to emphasize one point: the patterns that I’m about to discuss–at least some of them–are perfectly natural and normal. For the most part, there is nothing inherently wrong with these patterns, and hence no reason to pre-determine that they need to be “fixed”. It is only when we become so engrained in these patterns that we can’t get out of them–analogous to, and as I will explain actually connected to, the inability to vary autonomic states–that problems can arise. My point is that just because a person is in a certain pattern does not mean we need to mess with that pattern. And it’s also important to note that not all pain and injuries are a result of these patterns. Pain is a complex and relatively poorly understood phenomena (although there’s a lot of great research being done and published), but it is unquestionably a multifactorial issue; I highly recommend doing some reading on the biopsychosocial model of pain if you’re not already familiar with it.
Neurological and Anatomical Asymmetries of the Human Body
While humans may look pretty darn close to symmetrical to the naked eye (although this is not exactly the case, as I previously explained), if we delve beneath the surface and examine the internal makeup of the body it becomes apparent that there are numerous differences between our left and right sides. Anatomical asymmetries include:
- a heart and pericardium that is present on the left side but not on the right
- more lobes of lung on the right side than the left
- a hemidiaphragm that is larger, has a more optimal dome shape, and possesses more crural attachments (attachments to the spine) on the right side than the left
- a liver that is present on the right side but not the left
Neurological asymmetries include:
- lateralization of the brain (research suggests that the left hemisphere, which controls the right side of the body, is dominant in motor planning regardless of hand dominance)
- an imbalance between the right and left sides in positional sense and proprioceptive awareness, especially at the hip joint
The net effect is a bias towards the right side, which usually presents as a tendency to shift our weight onto our right leg when standing and our right ischial tuberosity (“sit-bone”) when sitting. This is the proverbial starting point for a sort of “chain reaction” that will result in compensations at the different joints in terms of posture and movement. Before I describe those compensations, however, I first need to explain PRI’s concept of polyarticular chains.
It’s All Connected: The Polyarticular Chains of Muscle
If you are familiar with fascia–the “sheath” that encloses our muscles–then you might already understand that our muscles aren’t really isolated units that work individually, but rather are interconnected in chains such that each muscle influences the other muscles in that chain. PRI teaches that the body can be divided into four different types of chains of muscle, with each present on both the right and left sides (technically making eight total chains). The four types of chains are as follows:
-The Anterior Interior Chain (AIC) consists of the diaphragm, psoas, iliacus (these two are treated as separate muscles, as opposed to one iliopsoas muscle), tensor fascia latae, vastus lateralis, and biceps femoris. The AIC can be visualized more simply as the muscles on the anterior side of the body from the knees to just above the bottom of the ribcage, excluding the abdominal musculature. These two chains (again, one on the right and one on the left) influence trunk rotation, hip flexion, as well as movement of the ribcage and spine. Due to the aforementioned asymmetries in the human body, the left Anterior Interior Chain tends to be more active than the right; people presenting with this pattern (aptly called the Left AIC pattern) have a right-sided bias in their lower body. In more precise terms, the AIC is responsible for ipsilateral swing phase and thus drives the transition to contralateral stance phase, so those with a Left AIC pattern tend to get stuck in right stance. It is also possible to have the Left AIC pattern bilaterally (the right hip’s position would mirror that of the left); these people are said to have a PEC pattern (addressed further below).
-The Brachial Chain (BC) consists of the anterior and lateral intercostals, deltoids, pectorals, Sibson’s fascia, triangularis sterni, sternocleidomastoid, scalenes, and the diaphragm (the diaphragm is included in multiple chains and can be considered the “most important” muscle in the PRI model, as it sort of ties the chains together). The BC can be visualized more simply as the muscles on the anterior side of the body from the neck down to the bottom of the ribcage. These two chains influence cervical rotation, shoulder movement, and expansion of the chest and ribcage. The BC on one side works in tandem with the AIC on the contralateral side; since the Left AIC is more active, we thus tend to see the Right BC pattern as the most common presentation. It is also possible, much like the AIC, to have the Right BC pattern on both sides (the position of the right ribcage and left scapulothoracic complex would mirror that of the left ribcage and right scapulothoracic complex, respectively); such people often also present with a PEC pattern and are said to have a Bilateral BC pattern.
-The Posterior Exterior Chain (PEC) consists of the latissimus dorsi, quadratus lumborum, posterior intercostals, serratus posterior, multifidus, spinalis longissimus, semispinalis fascia and muscle, and iliocostalis lumborum. The PEC can be visualized more simply as the muscles on the posterior side of the body from the top of the pelvis up to the neck. These two chains influence the position of the spine, pelvis, and ribcage and act in opposition to the BC’s and AIC’s. Because the precipitating cause of a person transitioning from having the Left AIC pattern on one side only to having it on both sides tends to be their use of the back musculature (or PEC) to achieve right trunk rotation (since the muscles normally responsible are in a compromised/mechanically disadvantageous position), such people are said to have a PEC pattern.
-The Temporal-Mandibular-Cervical Chain (TMCC) consists of the longus capitis, obliquus capitis, rectus capitis posterior major, rectus capitis anterior, temporalis (anterior fiber), masseter, and medial pterygoid. The TMCC can be visualized more simply as the muscles of the head and neck. These two chains influence cervical rotation, extension, and lateral movement, as well as orientation of multiple bones of the face and skull. The TMCC is covered in PRI’s secondary courses, and thus can be considered as more “advanced” material. As such, I will not cover it to any great extent in this series.
The “Chain Reaction”, and the Second Commandment of PRI: Thou Shalt Treat Muscles as Effectors of Movement in All Three Planes
As I previously explained, the natural anatomical and neurological asymmetries of the human body dictate that, to some degree, we have a bias towards our right side. This causes a tendency to “sink into” our right hip, which manifests as the lumbosacral complex rotating to the right. The net effect is a right hip that is positioned in a state of relative extension, internal rotation, and adduction, and a left hip that is positioned in a state of relative flexion, external rotation and abduction. These positions are typical of a Left AIC pattern; a person with a PEC pattern would essentially have a right hip position that mirrors the left (flexion, external rotation, and abduction).
Since the pelvis is oriented to the right, in order to stay facing forward we need to compensate by rotating the trunk back to the left. The net result generally includes:
- a right ribcage that is in a state of relative internal rotation and depression
- a left ribcage that is in a state of relative external rotation and elevation
- a right scapula that is relatively anteriorly tipped, protracted, and depressed
- a left scapula that is relatively posteriorly tipped, retracted, and elevated
These positions constitute the typical Right BC pattern. A person with a Bilateral BC pattern would have a right ribcage position that mirrors the left (externally rotated and elevated) and a left scapula position that mirrors the right (anteriorly tipped, protracted, and depressed).
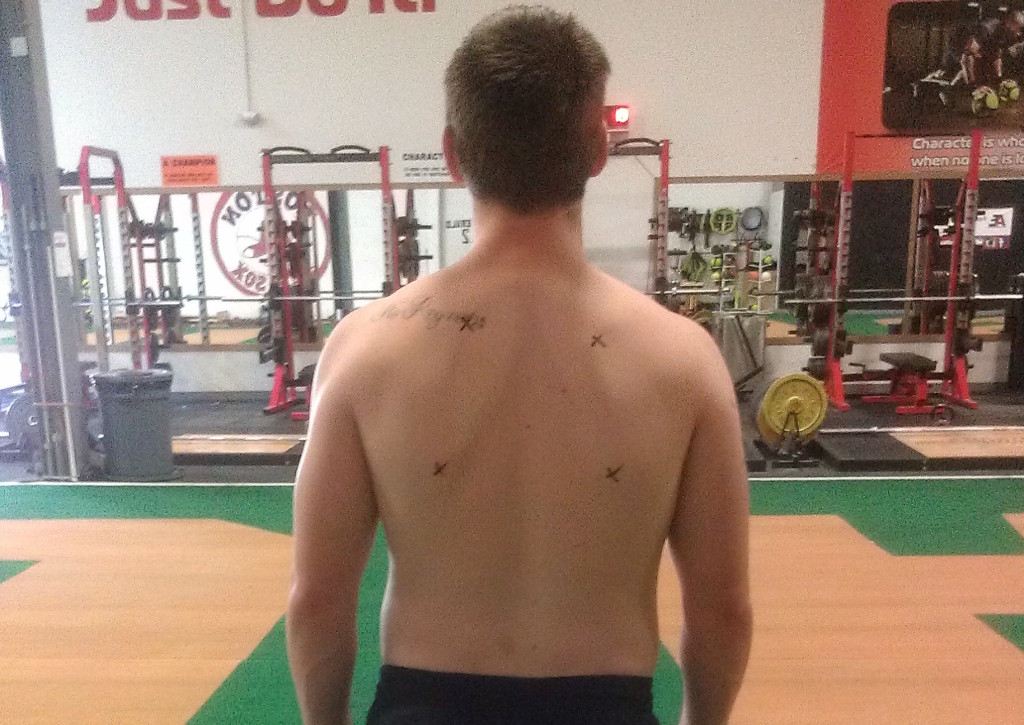
It’s important to note that one pattern can actually underlie another: since the Left AIC and Right BC patterns can be considered essentially inherent due to our natural asymmetries, even if someone develops a PEC and/or Bilateral BC pattern they may still have underlying Left AIC/Right BC tendencies. For example, while we would expect someone with a PEC pattern to be in chronic hip flexion on both sides, it is possible and actually fairly common for the left hip to be flexed to a greater degree than the right, as we would expect in a Left AIC pattern. Keep in mind, however, that all of these patterns, positions, and compensations can exist along a spectrum; that is, the degree to which these patterns exist can vary from individual to individual and is absolutely influenced by external factors specific to the individual’s lifestyle. I will address this concept in a later post.
The chronic positioning of these joints can have an effect on the resting length of the muscles that cross that joint. If the left hip is in a chronic state of flexion, for example, then the hip flexors will be put in a shortened state. I’ll cover ways of addressing specific patterns and muscles in my next post, so I’m not going to list and describe the common/expected resting state of every muscle. One aspect of this model that is worth noting, however, is what I call the Second Commandment of PRI: muscles must be considered as having an effect on movement in all three planes, even if they are a prime mover in a single plane. The gluteus maximus, for example, can be considered as a prime mover in the sagittal plane via extension of the hip joint, but it also contributes to external rotation and abduction (upper fibers specifically) of the hip. Thus, a person with the common chronic positioning of the hip joint seen in a Left AIC pattern would want to train the gluteus maximus on both sides, but in different planes: the left glute max should be trained in the sagittal plane via hip extension to counter the chronic hip flexion, and the right glute max should be trained in the transverse plane via external rotation and the frontal plane via abduction to counter the chronic internal rotation and adduction, respectively. Again, I’ll talk about this more in Part 4, but I want you to have an understanding of the relationship between chronic joint position and muscle length, as well as the triplanar approach to conceptualizing the effect muscles have on movement.
Piecing it All Together: Integration of Neurophysiology and Biochemistry
To this point, I’m sure Part 3 seems like a complete departure from Part 1 and Part 2. They are, however, all connected, and so getting through the at-times technical and tedious first two installments will indeed prove to be worth it (I hope)!
Recall that the neurological and biochemical mechanisms I outlined in Part 1 and Part 2 were responses to a stress or perceived threat. More specifically, stress is interpreted by the limbic system of the brain as a threat to our health and survival and as a result activates certain physiological responses mediated by the sympathetic division of the Autonomic Nervous System. With regards to posture and movement, there is evidence (laid out in Part 1 and Part 2) to suggest that sympathetic nervous system activation can affect skeletal muscle via increasing its resting tone and rigidity and decreasing its resting length.
But what does a stress response by skeletal muscle have to do with PRI and its application to treating and training people? It has been postulated that the right-side dominance that I described earlier in this piece is actually a survival mechanism in and of itself: in fight or flight situations, having a dominant/preferred side of the body in terms of muscle activity and movement allows the brain to avoid taking the minuscule but potentially life-saving amount of time to pick which side to react with. Since, as I’ve previously mentioned, physiological responses are fairly constant regardless of the nature of the stress or threat, it seems logical that shifting to our right side has simply been built in as a part of the sympathetic-driven stress response.
Also recall that, from a biochemical standpoint, it is likely that the muscles that are most affected by the stress response—and thus possess the aforementioned characteristics of high resting tone and rigidity as well as shortened length—are the muscles that have the highest metabolic demand, i.e. the ones that are used to the greatest extent. And if the stress response dictates that we shift to our right side when stressed or threatened, that is absolutely going to create a side-to-side as well as a front-to-back disparity between muscles in terms of usage/metabolic demand, especially if this response is chronically active. Thus, a pattern of neurological activity—which I like to define in this context as “the body’s way of reinforcing a response that promotes survival”—gives birth to and reinforces a pattern of muscle activity, posture, and movement.
Wrapping Up: Practical Implications
I’d be remiss (and you’d probably be a bit annoyed) if I didn’t discuss the practical applications of these postural and movement patterns and their connection to stress-driven and ANS-mediated neurological patterns. Here are a few that I consider to be relevant and important:
—Injury Reduction: I’d first like to note that I deliberately chose the term “injury reduction” over the often used “injury prevention”. Realistically speaking, there’s no way to “prevent” injuries—unfortunately, things that are outside of our control can and do happen no matter how much or how well you prepare, train, etc. As clinicians and coaches, the goal should be to put the client in a figurative and sometimes literal position that makes them less vulnerable to those events and thus minimizes their risk of injury.
PRI’s methodology can indeed play a large role in achieving this goal: postural and movement patterns that create side-to-side and/or front-to-back disparities in terms of muscle activity also create disparities in the wear-and-tear on those muscles, the connective tissues that sheath them and connect them to bone, as well as the connective tissues that make up the joints that these muscles cross and move. Teaching a client to “get out of” such a pattern and bringing them more towards a neutral position can reduce this wear-and-tear disparity, thus also helping to reduce the risk of injury.
—Neuropsychological/Stress Management Aid: In these first three installments, I’ve established that chronic activation of the stress response of the ANS drives physiological responses (primarily via the cardiorespiratory systems) that can lead to specific patterns of muscle activity, posture, and movement. While the most obvious and probably most effective way of resolving this situation and mitigating this response would be to remove the stress altogether, in today’s world this is not plausible more times than not. We are thus forced to look for alternatives, and PRI provides one: becoming better at coping with and responding to stresses and threats. Stephen Porges’ Polyvagal Theory states that an inability to successfully remove or mitigate a stress or threat results in “falling back” on a more primitive response; for example, chronic stress can cause us to abandon prosocial and self-soothing responses and fall back on the sympathetic-driven fight-or-flight response. If we focus on reinforcing those prosocial responses, however, and “teach” our body to get out of a sympathetic-dominant state, then we can essentially make ourselves into better copers in the sense that we are able to respond to chronic stress that is less taxing on our bodies and more conducive to good overall long-term health. PRI does exactly that: it attempts to counter the physiological manifestations of the stress response (increased cardiorespiratory activity, specific patterns of musculoskeletal activity) via focusing on breathing and muscle facilitation/inhibition in order to move us out of a sympathetic-driven response to stress and to promote a response that is more neutral in terms of the balance of ANS activity.
—Performance Enhancement: In order to optimize performance in the gym or on the field of play, an athlete must be able to maintain both neurological and musculoskeletal variability, being able to shift into and out of both neurological states as well as different movement patterns and postural positions as quickly and efficiently as possible. From a neurological standpoint, an athlete going 100% during a game needs to be able to “switch over” to a more parasympathetic-dominant recovery mode as soon as they take a rest, so that they are optimally prepared to perform when they return to play. From a musculoskeletal standpoint, if an athlete is “stuck” in a pattern that includes chronic hip flexion, then their ability to achieve full hip extension may be compromised; this could result in a decreased ability to produce power in movements as basic as running, and/or lead the athlete to compensate by getting that range of motion and power from another joint (perhaps the lumbar spine in the case of the hips) that isn’t necessarily equipped to handle that added stress. As I’ve already outlined under the previous two applications, PRI addresses and can help to improve both of these abilities.
That’ll do it for Part 3. In Part 4, I’ll go into greater detail on the postural patterns that PRI identifies, methods of addressing these patterns, and more specifics about the practical applications I introduced above.
Author’s Note: I would like to thank all of the wonderful PRI faculty members I have had the opportunity to learn from so far: James Anderson, Lori Thomsen, Jen Poulin, and Mike Cantrell. Their knowledge is only exceeded by their desire to help others learn the science of PRI and become better practitioners and coaches; I am extremely grateful for their help and guidance. I would also like to thank Eric Oetter, who first recommended Stephen Porges’ book to me and whose insight has helped to solidify my understanding of the neurophysiology underlying threat appraisal and response. Without all of you, these articles would not have been possible!

4 comments for “An Introduction to the Postural Restoration Institute, Part 3: The Asymmetrical Nature of the Human Body”